
Medicare has seemed to take over or even scare the physical therapy profession into only utilizing the 8-minute rule. As of today, the common way to bill units of physical therapy services in the outpatient setting is the 8-minute rule. However, there is another method that can be used to bill commercial insurance that predates the CMS 8 minute rule. This method is substantial portion methodology (SPM). Under the right circumstances, you can actually bill more units and, in turn, make more money using SPM.
If you're young in the profession, you may not have heard of this method. Even if you've been a practicing clinician for a number of years, you may have neglected SPM to make life easier or you may have forgotten about SPM altogether due to how your company bills insurances. If you are a practice owner or in a managerial position, I encourage you to look further into SPM. Under the right circumstances, you can actually bill more units and make more money to protect your bottom line using SPM.
SPM: Substantial Portion Methodology
SPM is not new! It actually predates the 8-minute rule. Before the 8-minute rule, SPM is how services were billed to all patients, including Medicare beneficiaries.
The SPM source of information is the Current Procedural Terminology (CPT) Assistant. The purpose of this text is to give advice on how to use and interpret CPT codes from the perspective of the AMA. Per the CPT Assistant, payers are within their rights to issue payment policies for reporting 97000 timed codes either following Medicare's guidelines or more strict guidelines. Payers are also given the latitude to request documentation supporting the medical necessity of a given portion of care provided within the 15-minute service descriptor.
While many private payers follow Medicare's rules, there are also several who issue individual reporting and billing guidelines. Some of these will accept substantial portion methodology.
What makes SPM different?
With timed codes, the "substantial portion" aspect of SPM means that the 15 minutes coded must be spent in performing the service described. That means performing what the CPT Assistant identifies as "pre-, intra-, and post-service work" of the code used.
For example, if a PT is performing manual therapy for a small fraction of the 15-minute period required to bill the service unit, that service unit should not be billed.
SPM examples for modalities:
- Iontophoresis (does not change): you can charge for everything except run time
- Ultrasound, attended e-stim, contrast bath, hubbard tank (does change): the prep and clean-up part of "pre, intra- and postservice work" is included in the charge
SPM only applies to timed codes
Nothing changes with service-based/un-timed codes.
- Serviced based/untimed codes - nothing changed from 8-minute rule:
- Do not require direct 1 on 1 time with the patient
- Can only bill one unit of each untimed code daily per discipline per patient (patient starts w/ hot pack and ends w/ cold pack = 97010 x 1)
- Allowed to double book timed and untimed codes
- Timed Codes- SPM only applies to timed codes:
- Any unskilled therapy is NOT covered
- Must be 1 on 1 with the patient
- Dressing changes still not covered
- Specific time of treatment must still be documented
- Co treatments and re-checks remain the same as with the 8-minute rule
Can a facility bill differently to payer sources for the exact same service?
Medicare does not set the rules for other payer sources. Facilities should follow payer guidelines in that payer's contract. If the contract is silent on specifics for timed codes, SPM set forth by the CPT assistant should be considered as a foundation for code selection.
Every payer can dictate how they choose to pay for physical therapy services. Medicare requires facilities to bill all Medicare patients according to the Centers for Medicare and Medicaid Services (CMS) 8-minute rule. However, the 8-minute rule is a Medicare rule, not a requirement that all payer sources are required to bill services by.
Billing breakdown: 8-minute rule vs. SPM
Payers who can be billed according to SPM:
- Blue Cross Blue Shield
- Aetna
- Cigna
- Auto (Geico, State Farm, Allstate)
- Workman's Comp
The sources who require physical therapy be billed according to the 8-minute rule:
- Medicare
- Medicaid
- Other Federal Payers:
- Tricare (Armed Services)
- Blue Cross for Federal employees
- Champus (veteran's)
- OWCP: Office of Worker's Compensation Program, administered by ACS
- Medicare Advantage Programs
- Medicare Plus Blue
- Pyramid Life
- Humana (advantage programs)
- Aetna Advantage Plans
Primary vs secondary payers:
- If either payer is a federal payer, bill according to the 8-minute rule.
Choosing between the 8-minute rule and SPM (for commercial insurances)
Scenario 1
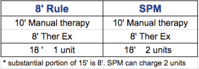

- If you're in a contract with Medicare, you cannot charge less for a service than what Medicare will reimburse. When a commercial insurance pays for therapy services, the numbers must be run both ways:
- Determine the number of minutes provided for each separate CPT (10 minutes manual therapy, 8 minutes ther ex)
- Run the numbers both ways
- Apply the most appropriate billing method
Scenario 2
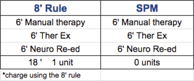

- Using the 8-minute rule, the patient will be charged 1 unit
- Using SPM, the patient would not be charged since none of the CPT codes were greater or equal to 8 minutes
- Since no single unit is greater than or equal to 8 minutes, the codes must be totaled, and the 8-minute rule will be applied to bill the correct charge.
- With commercial insurance, billing methods may vary from one session to another depending on the treatment provided (for example, the patient is billed according to the 8-minute rule on Tuesday, then billed according to SPM on Thursday)
Scenario 3
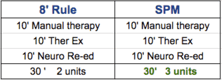
- 8-minute rule: apply greater skill principle and charge 2 units
- SPM: Manual x 1 , Ther Ex x 1 , Neuro Re-ed x 1 = 3 units
Scenario 4
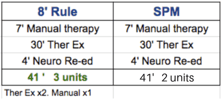
- Manual therapy and NRE codes are less than 8 minutes. The codes must be totaled and the 8-minute rule can be applied.
Scenario 5
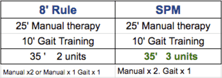
A substantial portion of the 30 minutes was utilized performing manual therapy, therefore it is appropriate to bill manual therapy x 2:
- 25 minutes - (15 minutes, 1 unit) = 10 minutes
- 10 minutes > 8 minutes
- 8 minutes = substantial portion of 1 whole unit of 15 minutes
- Bill Manual x 2 and Gait x 1
The moral of the story? Billing is complicated, but you do have options
In physical therapy school, we don't get very much instruction on how billing and coding works. Even as seasoned practitioners, billing and coding remain the most frustrating aspect of our jobs. But knowing the difference between SPM and the 8-minute rule—not to mention the other unique guidelines of physical therapy billing and coding—can help a practitioner deliver the best care to our patients and get paid appropriately for doing so.
Right now, many of us are considering telehealth opportunities. Here's what you need to know about telehealth billing codes.
